ROTTEN TEETH
Causes, Stages, Symptoms, Health Risks, Treatment Options & When to Act
Rotten teeth — clinically known as severe tooth decay or dental caries — are one of the most searched and most misunderstood dental topics. People want to know what rotten teeth look like, whether they can make you sick, what they smell like, and whether they can be fixed or saved. This article answers every major question clearly, honestly, and without promoting any product or provider. Whether you are dealing with rotten teeth right now or trying to prevent them, here is everything the evidence says.
| 📌 | Key fact: Rotten teeth are not a cosmetic problem. Untreated tooth decay progresses through the enamel and dentin into the pulp, creating an active bacterial infection inside your jaw. That infection can — and in documented cases does — spread to the throat, jaw, bloodstream, heart, and brain. This is a medical issue, not just a dental one. |
1. What Are Rotten Teeth? Definition and Medical Term
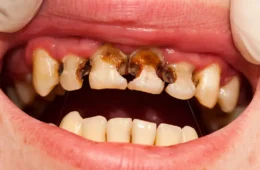
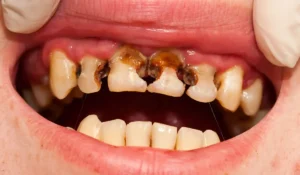
The medical term for rotten teeth is severe dental caries or advanced tooth decay. “Rotten” is a lay term — it simply means teeth that have decayed beyond the early cavity stage, with visible structural damage, discoloration, and often pain or infection. What do rotten teeth look like? In the early stages, they appear as white chalky spots or yellow-brown staining on enamel. In advanced stages, rotten teeth turn brown or black, develop visible holes and pitting, and can crumble or break at the gumline.
Rotten black teeth are at the most advanced visible stage — the black color indicates the decay has penetrated deeply through multiple tooth layers and may have reached the pulp. Rotten teeth at the gumline often indicate decay that began under the gumline or spread downward from the crown, and these are typically the most structurally compromised.
2. What Causes Rotten Teeth?
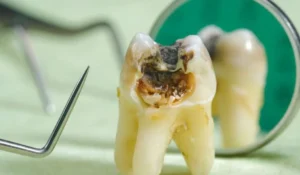
Causes of Rotten Teeth
Tooth decay does not happen overnight. It is a progressive process driven by several interacting causes. Understanding them is the only honest way to prevent it.
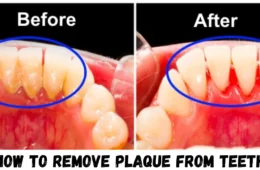
- Poor oral hygiene: The primary cause. When teeth are not brushed and flossed consistently, plaque — a sticky bacterial biofilm — accumulates on all tooth surfaces. Bacteria in plaque metabolize sugars and release acids that erode enamel. Learning the correct technique is essential — follow this step-by-step guide on how to brush your teeth properly to effectively remove plaque and protect your enamel.
- A diet high in sugar and refined carbohydrates: Sugary foods, candy, sweetened drinks, and refined starches feed the bacteria responsible for tooth decay. Rotten teeth from eating candy or sugar are particularly common in children and adults who consume high-sugar diets without adequate oral hygiene.
- Dry mouth (reduced saliva): Saliva neutralizes acids and washes away food debris. Medications, certain health conditions, mouth breathing, and dehydration all reduce saliva flow, significantly increasing decay risk.
- Genetics: Are rotten teeth genetic? Yes — partially. Enamel thickness, tooth shape, saliva composition, and immune response to oral bacteria all have genetic components. Some people are demonstrably more susceptible to tooth decay than others even with similar habits.
- Rotten teeth from drugs: Methamphetamine causes severe dental destruction — commonly called ‘meth mouth’ — through a combination of dry mouth, acidic pH, teeth grinding, and neglected hygiene. Tobacco smoking also dramatically increases decay and gum disease risk.
- Rotten teeth from braces: Orthodontic brackets create additional surfaces for plaque to accumulate. Poor hygiene during orthodontic treatment can cause rotten teeth after braces are removed, leaving white spot lesions or active cavities at bracket sites.
- Rotten baby teeth and rotten teeth in toddlers: Rotten milk teeth (also called baby bottle tooth decay or early childhood caries) occur when infants or toddlers sleep with milk, formula, or juice bottles. The sugars pool around teeth throughout the night. Rotten baby teeth, if left untreated, can damage the developing permanent teeth beneath them.
- Bulimia and stomach acid: Repeated exposure of teeth to gastric acid from purging causes severe enamel erosion, accelerating decay significantly. Rotten teeth from bulimia have a distinct erosion pattern affecting the inner surfaces of upper front teeth.
3. Stages of Rotten Teeth: From Early Decay to Total Destruction
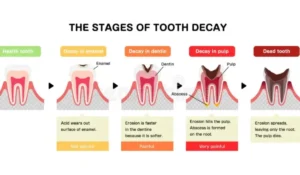
Stages of Rotten Teeth
Understanding the stages of tooth decay is critical — because treatment options and outcomes differ dramatically depending on the stage. The earlier decay is addressed, the less invasive and less costly the treatment.
| Stage | What’s Happening | What It Looks/Feels Like | Treatment at This Stage |
| Stage 1Initial demineralization | Acids begin leaching minerals from enamel | White or chalky spots — often no pain | Fluoride treatment may remineralize and reverse early decay |
| Stage 2Enamel decay | Enamel breaks down; cavity forms | Visible brown or white spot; mild sensitivity | Dental filling removes decayed area and restores tooth |
| Stage 3Dentin decay | Decay penetrates softer dentin beneath enamel | Increased sensitivity to heat, cold, sweet; visible hole | Filling or inlay; crown if damage is extensive |
| Stage 4Pulp infection | Bacteria reach the nerve and blood supply | Severe, throbbing pain; possible swelling | Root canal therapy to save the tooth; crown to restore |
| Stage 5Abscess formation | Infection spreads to root tip and jaw bone | Extreme pain, swelling, pus, possible fever | Root canal + antibiotics, or tooth extraction |
| Stage 6Advanced destruction | Tooth structure collapses; infection may spread beyond jaw | Black tooth fragments, loose teeth, systemic symptoms | Extraction; replacement with implant, bridge, or denture |
| ⚠️ | Rotten teeth early stages are the critical intervention window. At Stage 1 and 2, treatment is inexpensive, minimally invasive, and the tooth is fully saveable. By Stage 5–6, you are looking at root canals, extractions, and replacement costs of $1,500–$5,000 or more per tooth. An untreated $200 filling can evolve into a $2,000–$3,000 root canal and crown — or an emergency extraction. |
4. Symptoms of Rotten Teeth and Their Effects on Your Health
What Rotten Teeth Feel and Look Like
- Rotten teeth smell: Bacteria metabolizing decaying tooth tissue and food trapped in cavities produce sulfur compounds — the same compounds responsible for bad breath. Rotten teeth smell like poop or sewage in advanced cases because of anaerobic bacterial activity deep within the decay. The smell comes from the tooth itself, not from normal breath bacteria.
- Rotten teeth pain: Pain progresses from mild sensitivity at early stages to severe, constant, throbbing pain when the pulp is involved. When decay reaches the nerve, pain can radiate to the jaw, ear, or temple.
- Rotten teeth bleeding: Bleeding around a decayed tooth usually indicates gum disease or abscess formation — infection has spread to the surrounding gum tissue.
- Rotten teeth no pain: Some people with severely decayed teeth report little or no pain. This is not a sign the tooth is healthy — it can mean the nerve has died, which actually allows infection to progress silently and spread undetected.
Can Rotten Teeth Make You Sick? The Systemic Connection
This is the most searched question in this topic — and the answer is definitively yes. Rotten teeth can make you sick in multiple documented ways:
- Rotten teeth cause bad breath: Persistent bad breath (halitosis) is one of the most consistent signs of active tooth decay.
- Rotten teeth cause headaches and migraines: Dental infections create referred pain patterns that extend to the jaw, temples, and skull. Chronic dental infections have been linked to tension headaches and cluster headaches.
- Rotten teeth cause sore throat and throat problems: Bacteria from an abscessed tooth can track down the throat, causing pharyngitis or peritonsillar abscess — a potentially serious condition requiring medical intervention.
- Rotten teeth cause stomach problems: Swallowing bacteria-laden saliva from heavily infected teeth can disrupt gut microbiome balance, causing nausea, indigestion, and stomach discomfort.
- Rotten teeth cause sinus problems: The roots of upper back teeth lie close to the maxillary sinus. A decayed upper molar can infect the sinus lining directly, mimicking sinus infection symptoms — congestion, pressure, and post-nasal drip.
- Rotten teeth and heart disease: Oral bacteria can enter the bloodstream through inflamed gum tissue and infected tooth pulp. Research links chronic dental infection with atherosclerosis (arterial plaque hardening) and elevated heart attack and stroke risk. People with gum disease are four times more likely to develop rheumatoid arthritis.
- Rotten teeth cause high blood pressure: Systemic inflammation from chronic oral infection has been associated with elevated blood pressure in multiple population studies.
- Can rotten teeth kill you? Yes — in rare but documented cases. An untreated dental abscess can spread to the jaw (Ludwig’s angina), throat, chest, or brain. Sepsis (systemic blood infection) from a dental source is a documented cause of death. This outcome is rare with access to dental care but not hypothetical.
| 🚨 | Emergency signs: fever with tooth pain, significant facial or jaw swelling, difficulty swallowing or breathing, pus visible at the gumline, or extreme pain that prevents sleep — these are dental emergencies. Seek care immediately. A spreading dental infection can become life-threatening within days. |
5. How to Fix Rotten Teeth: Treatment Options by Stage
Rotten teeth treatment depends entirely on how far decay has progressed. Here is an honest overview of all available options, with realistic costs based on 2025–2026 US national averages.
| Treatment | When It’s Used | Approx. Cost (USA) | What It Achieves |
| Fluoride treatment | Stage 1 only — very early decay | $10–$75 | Remineralizes enamel; may reverse decay before a cavity forms |
| Dental filling | Stages 2–3 — cavity formed but decay hasn’t reached pulp | $100–$400/tooth | Removes decay; restores tooth shape and function |
| Dental crown | Stages 3–4 — extensive decay or post–root canal | $800–$1,500/tooth | Protects remaining tooth structure; full functional restoration |
| Root canal therapy | Stage 4 — pulp infected; tooth still salvageable | $300–$2,000/tooth | Removes infection; saves the natural tooth |
| Tooth extraction | Stages 5–6 — tooth beyond repair | $150–$650/tooth | Removes source of infection; prevents further spread |
| Dental implant | After extraction — permanent replacement | $3,000–$5,000/tooth | Replaces missing tooth with fixed, natural-feeling prosthetic |
| Dental bridge | After extraction — fixed replacement option | $1,500–$6,000 | Bridges the gap using adjacent teeth as anchors |
| Dentures (full or partial) | Multiple missing teeth | $600–$8,000 | Removable prosthetic replacing multiple or all teeth |
Can Rotten Teeth Be Fixed Without a Dentist?
This question gets enormous search volume — and deserves an honest answer. At Stage 1 (initial demineralization only), a very strict regimen of fluoride use, elimination of sugar, oil-rich diet, and improved hygiene can halt or partially reverse the earliest decay. This is the absolute limit of what home care can achieve. Once a physical hole or cavity has formed — Stages 2 through 6 — there is no legitimate home treatment that repairs the structural damage. The tooth cannot rebuild itself after enamel is lost. Herbal remedies, oil pulling, activated charcoal, and similar home treatments cannot restore tooth structure.
Attempting to scrape out decay with home tools risks permanent enamel damage, gum injury, and bacterial spread. Rotten teeth treatment at home has an honest role in prevention and in Stage 1 only — not in repair.
| ✅ | Can rotten teeth be saved? Yes — if treated early. Rotten teeth at Stage 1 and 2 are fully saveable with minimally invasive treatment. Even Stage 3 and 4 teeth can be saved with root canal therapy. Only Stage 5–6 teeth with structural collapse or severe bone loss require extraction. The earlier you act, the more options you have. |
6. Rotten Teeth in Children, Kids, and Toddlers
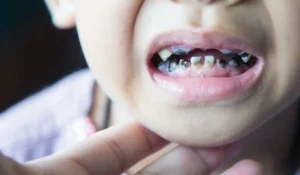
Rotten Teeth in Children
Rotten teeth in kids are alarmingly common. The WHO identifies dental caries as the most prevalent chronic disease in children worldwide. Rotten teeth in children most often result from a combination of high-sugar diets, infrequent brushing, and lack of professional dental care. Rotten baby teeth from not brushing, from excessive candy, from sleeping with bottles, or from chronic dry mouth all have the same consequence: bacterial acid erodes enamel faster in primary (baby) teeth because the enamel layer is thinner.
Do rotten baby teeth affect permanent teeth? Yes — directly. Untreated decay in a primary tooth can spread to the developing permanent tooth bud beneath it, infect the surrounding bone, and alter the eruption path of the adult tooth. This makes early treatment of rotten kids’ teeth essential, not optional. Many parents assume baby teeth do not matter because they fall out — this is a clinically dangerous misconception.
Rotten teeth in toddlers (2-year-olds and 5-year-olds especially) are a clinical emergency category because the decay can spread rapidly through thin primary enamel and reach the nerve in weeks. Rotten front teeth in toddlers are the most visible sign of early childhood caries and warrant immediate dental evaluation.
7. How to Prevent Rotten Teeth: The Evidence-Based Approach
- Brush twice daily with fluoride toothpaste: Fluoride is the single most effective tool for preventing tooth decay. Brush for two minutes, covering all tooth surfaces including the gumline.
- Floss once daily: Approximately 40% of all tooth surfaces are between teeth — only accessible by flossing. Interproximal (between-tooth) cavities are among the most common entry points for rotten teeth.
- Reduce sugar frequency — not just quantity: Every sugar exposure triggers a 20-minute acid attack on enamel. Sipping juice or soda throughout the day causes far more damage than drinking the same amount at one sitting.
- See a dentist every six months: Stage 1 and 2 decay is frequently painless and invisible without professional examination and X-rays. Regular checkups are the only reliable way to catch rotten teeth early stages before they become expensive and painful.
- Use fluoridated water: Community water fluoridation reduces childhood tooth decay rates by up to 25%, according to the CDC.
- Ask your dentist about dental sealants: Sealants applied to the grooves of back teeth prevent food and bacteria from collecting in the most decay-prone areas. They are particularly effective for children and teens.
Official Source: National Institute of Dental and Craniofacial Research — Tooth Decay (nidcr.nih.gov) — The NIH’s primary research institute on dental disease, cavity statistics, and treatment guidance
8. Frequently Asked Questions About Rotten Teeth
Q: What do rotten teeth look like?
A: Rotten teeth progress through visible stages. Early rotten teeth show as white chalky or yellow-brown spots on enamel. As decay advances, the tooth develops visible holes, pitting, and discoloration that deepens from brown to black. Rotten black teeth represent advanced decay that has penetrated through enamel and dentin. Rotten teeth at the gumline often appear as dark discoloration or breakdown at the tooth-gum junction. In the most advanced cases, the visible tooth crown may crumble entirely, leaving only a root fragment.
Q: Can rotten teeth make you sick?
A: Yes — definitively. Rotten teeth harbor active bacterial infections that can spread beyond the mouth. Documented health effects include severe headaches and migraines from dental pain referral, sore throat and sinus infections from spread of upper-tooth infections, stomach problems from swallowing infected bacteria, systemic inflammation linked to heart disease and elevated blood pressure, and — in rare but real cases — life-threatening spread of infection to the jaw, chest, or bloodstream. This is why dental infections should never be ignored.
Q: What do rotten teeth smell like?
A: Rotten teeth produce a distinctive and persistent odor caused by anaerobic bacteria metabolizing decaying tissue. The smell ranges from a sour acid odor in early stages to a strong sewage or fecal-like smell in advanced decay. Rotten teeth that smell like poop indicate deep anaerobic infection where bacteria produce hydrogen sulfide and methyl mercaptan — the same compounds found in decomposing organic matter. This smell persists despite brushing because it originates inside the decaying tooth structure, not from the tooth surface.
Q: Can rotten teeth be fixed?
A: Yes — if caught early enough. Stage 1 decay (white spots, no cavity) can be reversed with fluoride and dietary changes. Stage 2–3 decay (cavity through enamel and dentin) is repaired with a dental filling. Stage 4 (pulp infection) can be treated with root canal therapy to save the tooth. Stage 5–6 (abscess or structural collapse) typically requires extraction followed by an implant, bridge, or denture. The critical point: rotten teeth can almost always be fixed, but the treatment becomes more complex, invasive, and expensive at every stage of delay.
Q: Can rotten teeth kill you?
A: In rare but documented cases, yes. A dental abscess can spread through the jaw and neck (Ludwig’s angina), causing airway obstruction. Spreading dental infections have caused sepsis (systemic blood poisoning), bacterial meningitis, and brain abscess — all potentially fatal conditions. These extreme outcomes are uncommon in people with access to dental care, but they are not hypothetical. Emergency room visits for dental infections in the US exceed two million annually, many preventable with earlier treatment.
Q: Do rotten baby teeth affect permanent teeth?
A: Yes. Untreated decay in primary (baby) teeth can spread through the surrounding bone to damage the developing permanent tooth bud beneath. The infection can alter the eruption path of the adult tooth, cause enamel defects in the permanent tooth before it even erupts, or require more extensive treatment once the permanent tooth arrives. Baby teeth also hold space for permanent teeth — their early loss from decay can cause crowding and misalignment of the adult dentition.
Q: Why do rotten teeth smell so bad?
A: The odor from decayed teeth is produced by anaerobic bacteria — microorganisms that thrive without oxygen — deep within the cavity. These bacteria break down proteins and organic tissue, releasing volatile sulfur compounds (VSCs) including hydrogen sulfide and methyl mercaptan. These are the same compounds responsible for the smell of decomposing organic material. The deeper and more advanced the decay, the stronger and more persistent the odor, because it is coming from inside the tooth structure where brushing cannot reach.
Q: What is the fastest way to fix rotten teeth?
A: The fastest fix depends on the stage. For a simple cavity (Stage 2–3), a composite filling appointment takes 30–60 minutes and immediately restores the tooth. For an abscessed tooth causing severe pain, a dentist will drain the abscess, may prescribe antibiotics, and schedule root canal or extraction. There are no legitimate instant home fixes for rotten teeth beyond Stage 1. The fastest route to resolution at any stage is prompt professional treatment — delay always makes the condition worse and the treatment more complex.
Q: Can rotten teeth cause headaches, sinus problems, and high blood pressure?
A: Yes to all three. Dental infection pain is frequently referred to the jaw, temples, and skull — producing headaches and migraines. Upper molar roots sit immediately below the maxillary sinus; infection in these teeth can directly inflame the sinus lining, causing sinus pressure, congestion, and pain indistinguishable from a sinus infection. Systemic inflammation from chronic dental infection has been associated with elevated blood pressure in multiple population studies. Treating the underlying dental infection often resolves these secondary symptoms.
Final Word: What to Do If You Have Rotten Teeth
Rotten teeth are a progressive medical condition, not a cosmetic inconvenience. They cause real pain, real systemic health consequences, and — if left completely untreated — real danger. But they are also one of the most treatable conditions in medicine when caught early.
If you have rotten or decayed teeth right now, the most important thing is to act. Every stage of delay converts a simpler, cheaper treatment into a more complex, more expensive one. A $150 filling today becomes a $2,000 root canal and crown in a year, or an extraction and implant at $4,000 in two years. The infection does not resolve on its own — it spreads.
If cost is a barrier, dental schools provide supervised treatment at 50–70% reduced fees. Community health centers (FQHCs) offer sliding-scale dental care. Many practices offer payment plans. The path to treatment exists for most people — the critical step is taking it.
Editorial Note
This article is educational and non-promotional. All information is based on synthesis from MedicineNet, Colgate Oral Health, Oral-B, NIH NIDCR, Cleveland Clinic, Family Dental Care AU, Harris Dental Associates, and peer-reviewed dental research. No specific products or providers are recommended. Consult a licensed dentist for personal diagnosis and treatment. Visit elitefixdenture.com for detailed information.
Medically reviewed by: Dr. Aziz Liaquat, DDS
Dr. Aziz Liaquat is a licensed DDS with clinical experience in restorative and prosthetic dentistry, specializing in treating advanced tooth decay and full-mouth rehabilitation cases.