10 WARNING SIGNS YOU MAY NEED A ROOT CANAL
An Honest, Dentist-Informed 2026 Guide: Symptoms, Urgency Levels, What Happens During Treatment & When to See a Dentist
| 🚨 | If you have facial swelling, a fever with tooth pain, a pus-filled lump on your gum, or pain so severe you cannot sleep — do not wait for a scheduled appointment. Go to a dental emergency clinic or hospital emergency department today. Untreated dental infections can spread to the jaw, neck, and airway (Ludwig’s angina), which is life-threatening. |
What Is a Root Canal and Why Does It Matter?
A root canal (officially called endodontic treatment) is a dental procedure that removes infected or damaged pulp — the soft tissue containing nerves, blood vessels, and connective tissue — from inside a tooth. The hollow space is then cleaned, shaped, and sealed to prevent reinfection. The tooth is preserved and typically capped with a crown.
Root canals have an undeserved reputation for being extraordinarily painful. In reality, the procedure itself is performed under local anesthesia and is generally no more uncomfortable than having a cavity filled. The pain people associate with root canals is the infection and inflammation that makes one necessary — not the treatment itself.
The critical point: a tooth that needs a root canal will not heal on its own. The pulp does not regenerate. Without treatment, the infection spreads — to surrounding bone, neighboring teeth, and potentially to the jaw, neck, and bloodstream. Early treatment is almost always less painful, less expensive, and less complicated than waiting.
| 📌 | Only a licensed dentist or endodontist (root canal specialist) can diagnose whether you need a root canal. This article describes the common warning signs to help you recognize when to seek professional evaluation — not to replace that evaluation. |
All 10 Warning Signs at a Glance
| Sign | Symptom | Urgency |
| #1 | Severe, throbbing toothache | 🚨 Emergency |
| #2 | Prolonged sensitivity to hot/cold | 🚨 See dentist soon |
| #3 | Facial or jaw swelling | 🚨 Emergency |
| #4 | Darkened or discolored tooth | ⚠️ Schedule check-up |
| #5 | Gum boil or pimple on the gum | 🚨 See dentist soon |
| #6 | Pain when biting or chewing | ⚠️ See dentist soon |
| #7 | Cracked or chipped tooth with pain | ⚠️ See dentist soon |
| #8 | Deep cavity or decay near the nerve | 📌 X-ray finding |
| #9 | Loose tooth in adults | 📌 Schedule check-up |
| #10 | Fever or bad taste/smell from tooth | 🚨 Emergency |
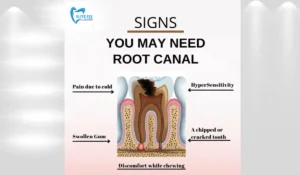
The 10 Warning Signs You May Need a Root Canal — Explained
WARNING SIGNS YOU MAY NEED A ROOT CANAL
| SIGN #1 | Severe, Persistent, Throbbing Toothache |
A deep, throbbing, or pulsing toothache that does not go away — especially one that wakes you at night or is not relieved by over-the-counter pain medication — is one of the most telling signs of pulp infection or death. This type of pain typically means the nerve inside the tooth is severely inflamed or infected. It is different from the temporary sharp pain of sensitivity: it lingers, intensifies, and may radiate to the jaw, ear, or temples. Severity alone is not the diagnosis — your dentist will use X-rays, percussion testing, and pulp vitality tests to confirm — but severe, persistent toothache warrants urgent evaluation, not watchful waiting.
| SIGN #2 | Prolonged Sensitivity to Hot or Cold |
Brief sensitivity to hot or cold food and drink is common and often benign, caused by exposed dentin or early enamel erosion. The root canal warning sign is sensitivity that persists — pain or discomfort that continues for 30 seconds or more after the hot or cold stimulus is removed. This lingering sensitivity, especially to heat, suggests that the dental pulp is inflamed (pulpitis). When sensitivity to cold lingers, it often indicates reversible pulpitis that may resolve; lingering sensitivity to heat more often signals irreversible pulpitis — meaning the pulp cannot recover and root canal treatment is likely necessary. If you need to avoid hot or cold food on one side of your mouth, see a dentist.
| SIGN #3 | Facial, Jaw, or Gum Swelling |
Swelling in the face, cheek, jaw, or under the chin — particularly swelling that is warm to the touch, progressively worsening, or accompanied by fever — is a dental emergency. It indicates a spreading infection that has moved beyond the tooth root into surrounding tissue. Mild gum swelling near one tooth may be localized and less urgent; significant facial swelling that changes the shape of your face, makes swallowing difficult, or is accompanied by fever requires same-day emergency treatment. Dental abscesses can spread rapidly — a condition called cellulitis — and can become life-threatening if infection reaches the airway or bloodstream. Do not take antibiotics alone and wait; the infection source must be treated.
| SIGN #4 | Darkened or Discolored Tooth |
A tooth that is noticeably darker than its neighbors — taking on a gray, brown, or black hue — may indicate that the pulp inside has died. Pulp death (pulp necrosis) can result from trauma (a blow to the tooth), severe decay that cuts off the blood supply, or a prior failed restoration. The discoloration occurs because hemoglobin from ruptured blood vessels in the pulp breaks down and penetrates the surrounding dentin. A darkened tooth is not always painful — dead pulp means no nerve sensation — which is why many patients with necrotic pulp have no pain until infection develops. A darkened tooth that you did not have a few months ago warrants a dental X-ray and evaluation, even if it feels fine.
| SIGN #5 | Gum Boil, Pimple, or Fistula on the Gum |
A small pimple-like bump, blister, or raised area on the gum near the base of a tooth — often called a gum boil or dental fistula (sinus tract) — is a classic sign of a dental abscess draining. The ‘pimple’ is an opening that allows pus from an infected tooth root to drain into the mouth. You may notice a bad taste or smell coming from it. A draining fistula can cause the acute pain to temporarily subside (as pressure is released), which sometimes misleads patients into thinking the problem has resolved. It has not. The infection source — the infected tooth root — is still present and still actively destroying surrounding bone. This sign always requires professional evaluation and treatment.
| SIGN #6 | Pain When Biting or Chewing |
Pain specifically triggered by biting down or chewing — particularly sharp or throbbing pain on one tooth — can indicate pulp inflammation, a cracked tooth exposing the pulp, or a periapical abscess (infection at the root tip). The periapical ligament surrounding the tooth root contains pressure-sensitive fibers; when an abscess forms at the root tip, even the light pressure of biting causes significant pain. This symptom can also indicate a cracked tooth syndrome (see Sign #7). Either way, pain triggered by biting or chewing that persists or worsens over more than a few days warrants professional examination — biting pain does not resolve on its own when the cause is pulpal or periapical infection.
| SIGN #7 | Cracked or Chipped Tooth with Pain or Sensitivity |
A visible crack or chip in a tooth is not automatically a root canal situation — small, superficial chips may only need bonding or a crown. The warning sign is a crack that extends down into the pulp chamber, or a chip accompanied by persistent pain, sensitivity, or swelling. Cracked tooth syndrome is a common and frequently underdiagnosed cause of root canal need: an incomplete crack that does not show on X-rays but causes sharp pain when biting in certain directions. If you cracked a tooth in an accident, had a large filling break, or ground your teeth aggressively, have it evaluated even if pain is mild — vertical root fractures are serious and can make the tooth unrestorable if caught too late.
| SIGN #8 | Deep Cavity Reaching Near or Into the Pulp |
A very deep cavity that approaches or penetrates the dental pulp is one of the most common causes of root canal need. Often identified on dental X-rays before symptoms appear, a deep cavity that has broken through the enamel and dentin into the pulp chamber introduces bacteria directly into the nerve space, leading to infection. The tooth may be symptom-free initially — which is why regular dental X-rays matter — or it may already be causing pain or sensitivity. If your dentist tells you a cavity is ‘very deep’ or ‘close to the nerve,’ do not delay treatment. A tooth caught at this stage with reversible pulpitis can sometimes be saved without a root canal; one allowed to progress to irreversible pulpitis or abscess almost always cannot.
| SIGN #9 | Loose Tooth in an Adult |
Adult teeth should not be loose. If a tooth has developed mobility — meaning it wiggles when you touch it — this can indicate severe bone loss from periodontal disease, an injury, or infection around the root that has destroyed the supporting bone and periodontal ligament. A necrotic (dead) tooth sometimes becomes loose because the infection at the root tip has dissolved enough surrounding bone to remove structural support. Looseness alone does not always mean a root canal is needed — a periodontist evaluation may be appropriate — but it always requires professional assessment. A loose adult tooth that is also painful, swollen, or associated with other symptoms on this list should be evaluated urgently.
| SIGN #10 | Fever, Bad Taste, or Foul Smell From a Tooth |
Fever associated with tooth pain is a serious warning sign that dental infection has become systemic — your body is fighting a bacterial infection that has spread beyond the tooth. A persistent bad taste (not related to food or drink) or foul smell from a specific tooth or gum area often indicates pus drainage from an abscess. These signs together — fever, bad taste, facial swelling — constitute a dental emergency. Antibiotics may be prescribed to reduce systemic infection before treatment, but antibiotics alone will not resolve the infected tooth pulp or abscess. Dental treatment — root canal or extraction — is required. Do not wait to see if the fever resolves.
Urgency Guide: When to Go Today vs. This Week vs. Schedule a Check-Up
Not every root canal warning sign is a same-day emergency — but some are. Use this guide to determine how quickly you need to act.
| 🚨 GO TODAY | ⚠️ CALL THIS WEEK | 📌 SCHEDULE CHECK-UP |
| • Facial or jaw swelling • Fever with tooth pain • Can’t swallow / open mouth • Severe uncontrolled pain • Pus draining from gum | • Lingering cold/heat sensitivity • Gum boil / fistula present • Pain when biting (daily) • Cracked tooth with symptoms • Loose adult tooth | • Darkened tooth, no pain • Deep cavity found on X-ray • Mild occasional sensitivity • History of trauma to tooth • Old large filling breaking down |
What Actually Happens During a Root Canal Procedure
Fear of root canals is largely based on outdated information. Modern endodontic treatment — performed by a dentist or endodontist using local anesthesia, rotary instruments, and digital X-rays — is a routine procedure for experienced practitioners.
Step 1 — Anesthesia: Local anesthetic (typically lidocaine) is injected around the tooth. Once numb, you should feel pressure but not pain. If you are anxious, conscious sedation options (nitrous oxide, oral sedation) are available at most practices.
Step 2 — Access opening: A small opening is drilled through the top of the tooth to access the pulp chamber and root canals.
Step 3 — Pulp removal: Tiny files remove the infected or dead pulp tissue from each root canal. The canals are shaped and widened to allow thorough cleaning.
Step 4 — Cleaning and disinfection: Antibacterial irrigants (usually sodium hypochlorite) flush bacteria and debris from the canal system.
Step 5 — Filling (obturation): The cleaned canals are filled with a biocompatible rubber-like material called gutta-percha and sealed with dental cement.
Step 6 — Restoration: A temporary filling closes the access opening. At a follow-up appointment, a permanent crown is placed — essential to protect the now-brittle treated tooth from fracture.
Total time: 60 to 90 minutes for a single-rooted tooth (front tooth); 90 to 120 minutes for multi-rooted teeth (molars). Complex cases may require two appointments. Post-procedure soreness for 2 to 4 days is normal and manageable with ibuprofen or acetaminophen.
| 📌 | Endodontists (root canal specialists) complete 2 to 3 additional years of training beyond dental school and focus exclusively on root canal procedures. For complex cases, severely curved canals, or previously treated teeth needing re-treatment, an endodontist referral is appropriate. |
Root Canal Cost in the USA: What to Expect
Front tooth (single root): $700 – $1,200 at a general dentist; $900 – $1,500 at an endodontist.
Premolar (one or two roots): $800 – $1,400 at a general dentist; $1,000 – $1,700 at an endodontist.
Molar (two to four roots): $1,000 – $1,800 at a general dentist; $1,200 – $2,200 at an endodontist.
Crown (required after root canal): $1,000 – $2,000 additional, depending on material and location.
Insurance coverage: Most dental insurance plans cover 50 to 80% of root canal costs after the deductible, up to your annual maximum. The crown may be covered under a separate restorative benefit.
| ⚠️ | Delaying a root canal does not make it cheaper — it makes it more expensive. An abscess that spreads may require antibiotics, hospital treatment, or extraction followed by an implant ($3,000–$5,000) or bridge ($2,500–$5,000). Early root canal treatment is almost always the least expensive option when a tooth is salvageable. |
Root Canal vs. Tooth Extraction: Which Is Better?
Many patients ask whether extraction (pulling the tooth) is a simpler, cheaper alternative to a root canal. The honest answer depends on the specific situation, but saving your natural tooth is almost always the better long-term outcome when possible.
- Natural teeth function better than any artificial replacement. Implants and bridges are excellent solutions, but they do not replicate the natural sensation of a real tooth.
- Tooth loss triggers bone resorption (jawbone shrinkage) at the extraction site, which accelerates over time and can affect neighboring teeth and facial structure.
- Extraction followed by an implant typically costs $3,000 to $5,500 — significantly more than a root canal and crown in most cases.
- Not every tooth is worth saving. A tooth with a vertical root fracture, severe periodontal bone loss, or insufficient structure for a crown may be better extracted. Your dentist or endodontist can assess restorability.
| ✅ | The American Association of Endodontists recommends saving natural teeth whenever clinically feasible. A root canal and crown on a restorable tooth is almost always preferable to extraction and replacement — both clinically and financially. |
Frequently Asked Questions
Q: What does a root canal feel like?
A: During the procedure, with proper local anesthesia, most patients feel pressure and vibration but not pain. The tooth and surrounding gum are fully numb. Any pain during the procedure typically means anesthesia needs to be supplemented — tell your dentist immediately so more anesthetic can be administered. After the procedure, 2 to 4 days of soreness and tenderness is normal, managed with over-the-counter anti-inflammatories.
Q: Can a tooth that needs a root canal heal on its own?
A: No. Once the dental pulp is infected or dead, it cannot regenerate or heal itself. The infection will continue to spread — to surrounding bone, neighboring teeth, and potentially systemically. Some patients experience temporary pain relief when an abscess ruptures and drains, but this does not mean the infection has resolved. Treatment is always required.
Q: How do I know if I have a tooth abscess?
A: Signs of a tooth abscess include: severe throbbing toothache, sensitivity to hot food or drink, facial or jaw swelling, fever, a pimple-like bump on the gum near the painful tooth, a foul taste or smell, and difficulty opening your mouth or swallowing. Mild abscesses may cause only gum tenderness and a gum boil. Severe abscesses with facial swelling, fever, or difficulty swallowing are medical emergencies.
Q: Is a root canal painful?
A: The procedure itself, performed under local anesthesia, is not painful for most patients — studies consistently show that root canal discomfort is comparable to or less than other routine dental procedures. The days before treatment — when infection and inflammation are at their peak — are usually the most painful. Post-procedure soreness is mild to moderate and temporary.
Q: What happens if I don’t get a root canal?
A: Without treatment, the infected pulp dies and the infection spreads to the periapical bone (around the root tip), forming a dental abscess. The abscess can spread to the jaw, face, and neck — a condition called Ludwig’s angina — which is potentially life-threatening. The tooth will eventually need extraction, after which bone loss begins at the extraction site. Delaying treatment always worsens the prognosis.
Q: Do I need a crown after a root canal?
A: For back teeth (premolars and molars), a crown is strongly recommended — nearly always required. These teeth bear the majority of chewing force, and the root canal procedure makes them more brittle and fracture-prone. Without a crown, a treated molar frequently fractures vertically and becomes unrestorable. Front teeth (incisors and canines) that have adequate remaining structure may be restored with a filling rather than a crown — your dentist will assess the remaining tooth structure.
Q: Can I eat normally after a root canal?
A: Avoid chewing on the treated tooth until the permanent crown is placed. Eat on the opposite side and avoid hard, crunchy, or sticky foods on the treated side. After the crown is placed and the area has fully healed (usually 2 to 3 weeks), you can resume normal eating.
Q: What is the difference between a root canal and a filling?
A: A filling addresses decay that has not yet reached the pulp — only the outer enamel and dentin are treated, and the nerve is preserved. A root canal is necessary when decay, infection, or trauma has reached or destroyed the pulp itself. Root canals are more complex, take longer, cost more, and require a crown afterward. A very deep filling that approaches the nerve sometimes transitions to a root canal if the pulp becomes inflamed or infected after treatment.
Final Summary: Don’t Ignore These Warning Signs
Root canal warning signs are your body’s communication that something is seriously wrong inside a tooth. The 10 signs covered in this article — from severe throbbing pain and facial swelling to darkened teeth and gum boils — all indicate that the dental pulp is infected, inflamed, or dead and that professional evaluation is needed.
The most important things to remember: early treatment is almost always less painful, less complicated, and less expensive than waiting. A tooth that needs a root canal will not get better on its own. And facial swelling with fever is a medical emergency — not something to treat with antibiotics and monitor at home.
If you recognize any of these signs, contact your dentist or endodontist for an evaluation. If you have swelling, fever, or severe uncontrolled pain, go to a dental emergency clinic or hospital emergency department today.
| ✅ | Key takeaway: Any toothache lasting more than 2 to 3 days, sensitivity that lingers after the hot or cold source is removed, or any visible gum boil or facial swelling warrants a professional dental evaluation — not home remedies or watchful waiting. Prompt treatment saves teeth, saves money, and prevents serious complications. |
Medical Disclaimer
This article is for informational and educational purposes only and does not constitute dental or medical advice, diagnosis, or treatment. Only a licensed dentist or endodontist can diagnose whether you need a root canal through clinical examination and diagnostic imaging. If you are experiencing tooth pain, swelling, or any symptoms described in this article, seek professional dental care promptly. In cases of facial swelling, fever, or difficulty breathing or swallowing, seek emergency medical care immediately.
Medically reviewed by:
Dr. Aziz Liaquat, DDS
Doctor of Dental Surgery
New York University College of Dentistry